 Sumyra Kachru, MD
Sumyra Kachru, MD
Gastroenterology
Orlando Health
Colorectal cancer (CRC) is the third most common cancer diagnosed in the United States. Nearly 1 in 3 people who develop colorectal cancer have a family history of the disease. The risk is even higher if you have someone in your immediate family — a parent or sibling — who has had CRC or colon polyps. Colorectal cancer usually develops from precancerous polyps in the colon or rectum.
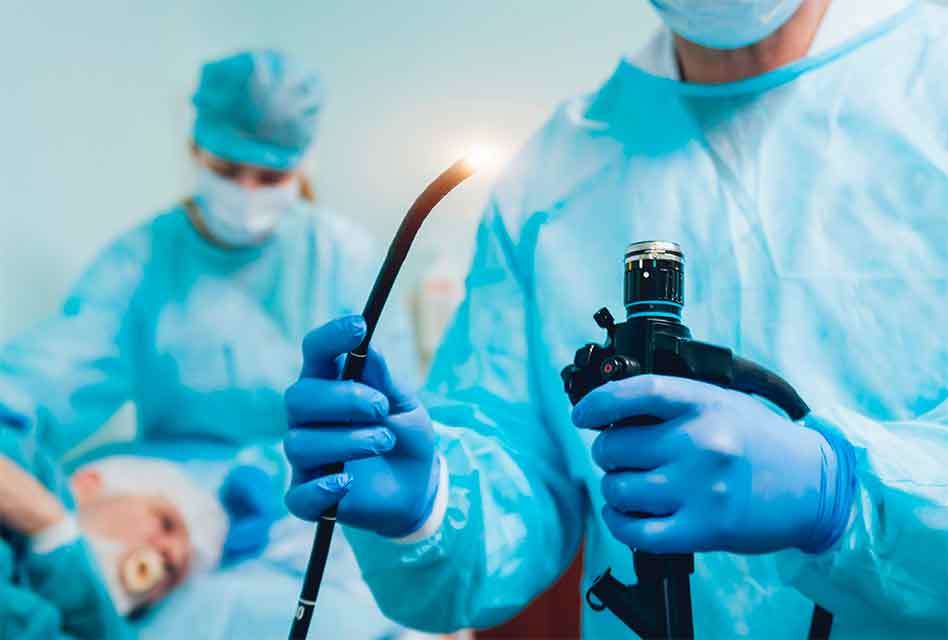
The first line of defense against CRC is a colonoscopy, which is recommended for everyone starting at age 45. Colonoscopies are used detect polyps and other colorectal issues such as ulcers. If you have a family history of colon polyps, getting regular colonoscopies is your best defense against developing colorectal cancer, as potentially cancerous polyps can be treated or removed following a colonoscopy.
What Are Colon Polyps?
A colon polyp is a small growth of excess tissue on the inner lining of the large intestine, also called the colon. Polyps may appear flat or as raised bumps (sessile) or may grow on short stalks like a mushroom (pedunculated).
There are five different types of colon polyps:
- Adenomatous (tubular adenoma). The most common type of polyp, this type can become cancerous. If you have a personal or family history of these polyps, you will need periodic colonoscopies to find and remove them.
- Hyperplastic. These are small polyps that have a low risk of turning cancerous. If a hyperplastic polyp is found, it will be removed and tested to ensure it is not cancerous.
- Villous adenoma (tubulovillous adenoma). This type of polyp has a high risk of turning cancerous. Smaller villous adenomas may be removed during a colonoscopy, and larger ones may require surgery for removal.
- Pseudopolyps (inflammatory). Most common in people with inflammatory bowel disease (IBD), this type of polyp occurs as a result of chronic inflammation in the colon. Inflammatory polyps do not turn cancerous.
- Serrated. These polyps are growths that stick out from the surface of the colon or rectum. Serrated polyps can be hard to detect and have a saw-toothed appearance when viewed under a microscope. They are precancerous and must be removed.
Most polyps are not cancerous, and it takes an estimated 10 years for a polyp to turn into cancer. Because most polyps don’t cause symptoms, regular colonoscopies are the best way to detect and remove polyps to prevent colorectal cancer.
How Family History Affects Colorectal Cancer Risk
Approximately 5 percent of people who develop colon cancer have inherited a genetic predisposition (gene mutations) that may lead to the disease. The most common inherited genetic conditions linked to colorectal cancer include:
Lynch syndrome. Also known as hereditary non-polyposis colorectal cancer (HNPCC), this is the most common cause of hereditary colorectal cancer, accounting for 2 to 4 percent of all cases. Lynch syndrome is caused by inherited mutations in certain genes. These genes normally help repair damaged DNA, but mutations in these genes can prevent them from working as they should.
Familial adenomatous polyposis (FAP). Caused by mutations in the APC gene, FAP causes hundreds of polyps to develop in a person’s colon or rectum by early adulthood. Almost every person with FAP will have colon cancer by age 40 if the colon is not removed. FAP accounts for approximately 1 percent of all colorectal cancer cases.
6 Ways To Protect Against Colon Cancer
Lifestyle habits related to diet, physical activity and body weight are also linked to the risk of colorectal cancer. Making positive lifestyle changes and sticking to healthy habits can be challenging, but these changes can lower your risk of developing colorectal cancer and other types of cancers and diseases.
- Eat a healthy, balanced diet full of fruits, vegetables, lean proteins and whole grains. Research shows a link between processed foods and red meats and an increased risk of colorectal cancer.
- Maintain a healthy body weight. Being overweight or obese increases the risk of developing colorectal cancer. Staying at a healthy weight may lower your risk.
- Reduce alcohol intake. Alcohol intake is associated with a higher risk of colorectal cancer, particularly in men.
- Stop smoking. Smoking is linked with an increased risk of many health problems and cancers, including colorectal cancer.
- Physical activity. Regular exercise (at least 150 minutes per week of moderate-intensity exercise or 75 minutes per week of vigorous exercise) can help lower your risk.
- Regular screening. Regular check-ups and screening tests are essential for early detection and prevention. Guidelines suggest that adults should have their first colonoscopy at age 45, and follow-up colonoscopies at regular intervals depending on what’s found during the initial screening. Individuals with a family history of polyps or colorectal cancer should begin screening at an earlier age and at more frequent intervals.
Warning Signs of Colon Polyps
Polyps generally do not cause any symptoms, and most people don’t know they have them until they’re detected during a colonoscopy. Large colon polyps may cause symptoms, including:
- Pain. Large polyps can lead to a bowel obstruction that causes abdominal cramping and pain.
- Bleeding. You may notice blood in the toilet or on your underwear after a bowel movement.
- Changes in stool color. Blood in the stool may make it appear black or streaked with red.
- Changes in bowel movements. Constipation or diarrhea that lasts a week or more.
- Weight loss. Unintentional weight loss may be a sign of colon polyps or colorectal cancer.
Being vigilant about your bowel health, regardless of family history, is the best way to protect against colorectal cancer. Talk with your doctor about your risk factors and screening recommendations.
Source: Orlando Health